



Standing hindfoot alignment view
Calcaneal valgus angle should be 5deg
Meary's angle (marked) should be <10deg
Dorsoplantar talo-first metatarsal angle (left) should be <10deg
Talonavicular coverage angle (right)
The diagnosis of adult acquired flatfoot is made clinically. If there is no controversy about diagnosis or management we do not routinely obtain radiographs. However, in many patients there is a need to assess the joints and alignment for treatment planning, and in some there may be the possibility of inflammatory arthropathy or a tarsal coalition.
The standard plain films are:
On these views we assess the following parameters:
 |
 |
  |
Standing hindfoot alignment view |
Standing lateral view. Meary's angle (marked) should be <10deg |
Standing dorsoplantar view. Dorsoplantar talo-first metatarsal angle (left) should be <10deg Talonavicular coverage angle (right) |
If we are planning surgery, or if there is any other need to assess the tendons and ligaments, we obtain an MR scan. Ultrasonography has also been described and is probably of equal accuracy to MRI, provided expertise and suitable equipment are available.
CT shows bony changes well, but does not show soft tissues clearly.
 |
| Transverse MRI showing split in tibialis posterior tendon |
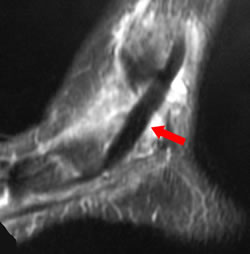 |
| Sagittal MRI showing thickened tibailis posterior tendon |
MR shows:
Conti et al (1992) classified the MR appearances:
Conti et al found that the MR appearances were a better guide to outcome than surgical findings. In particular tendon transfers were significantly more successful in type 1 tendons, but tendons graded type 1 by the surgeon were graded type 2 by MR in 10/17 patients - intra-operative assessment may lead to inappropriate choice of treatment.